For more information, please learn more about and support community-based sources like the Intersex Justice Project who “works to end invasive and unnecessary surgeries on intersex youth by empowering intersex people of color as change-makers.”
Please note before reading, the content below includes reference to historic medical trauma against intersex people.
(Biological Sex) Biological Characteristics of Sex
More than two “sexes” are commonly found throughout the animal kingdom, including up to 2% of humans. Many people have characteristics that do not easily fall into the category of “male” or “female” due to one’s genitals, gonads, and/or genetics, which may or may not be visible externally. Generally, this biocommunity prefers the term intersex (as in the “I” in LGBTQAI+) to being labeled as having a “Disorder/Variation of Sex Development” (D/VSD) — a recently taxonomized and unnecessarily pathological label often used to validate medical intervention.
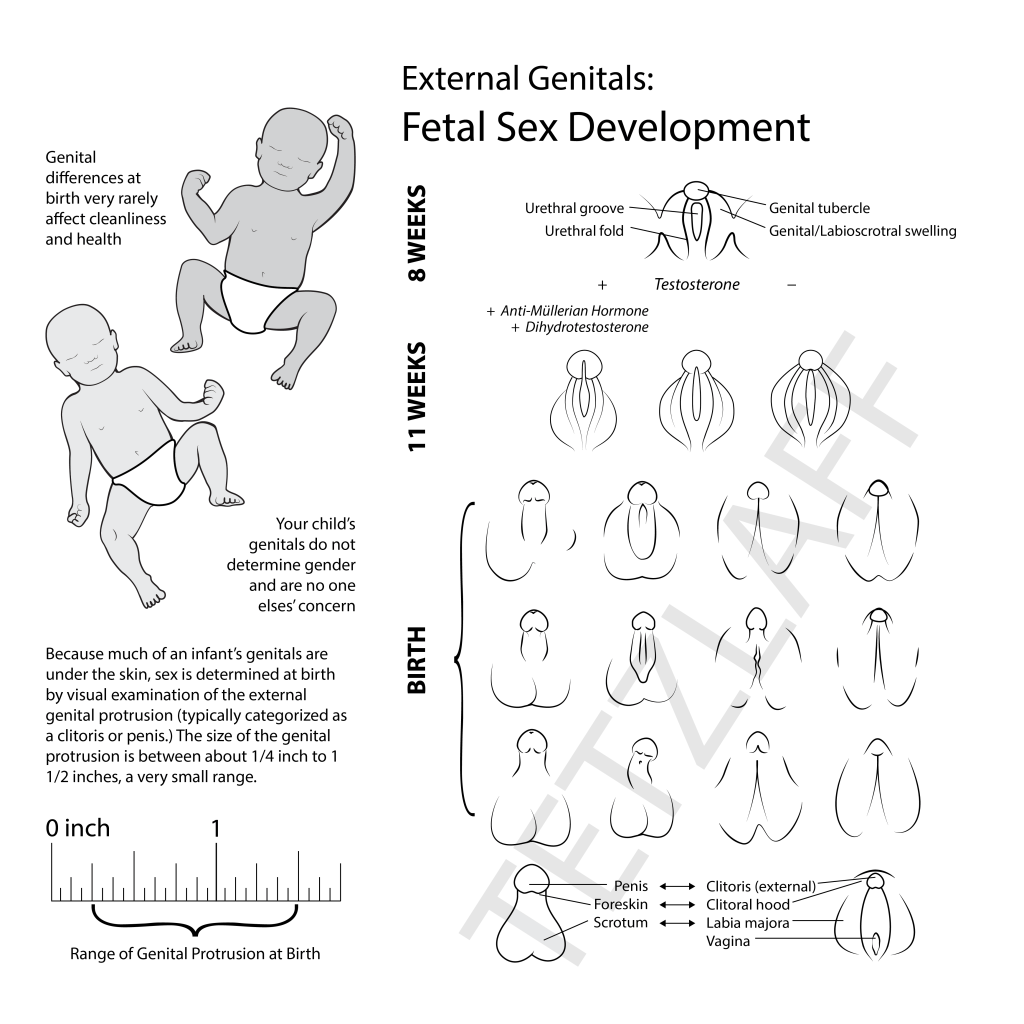
So what is sex and how is it determined? At birth, a doctor assigns the infant a sex, and therefore a gender, based on the appearance of the external genitals. Assigning sex does not typically involve chromosomes, gonads, hormone prevalence, etc. — and it doesn’t include gender identity that starts to develop around age 4. “Sex” is largely a social construct. Virtually no one has genetic testing to determine chromosome type; or a gonadal biopsy to classify tissue types; or a hormone test at birth and again at puberty; etc. For these reasons, sex is not a biological constant, far from it. Therefore, it is more accurate to refer to biological characteristics of sex, rather than “biological sex.”
With rare exception, intersex characteristics are not life-threatening. Despite this, parents of intersex children are often pressured by a team of physicians to submit their child to genital “normalization” surgeries, which are often kept as a secret from the child that can engender shame. However, intersex activists like Sean Saifa Wall, Pidgeon Pagonis, Caster Semenya, Emily Quinn, Georgiann Davis, and Small Luk are making progress around the world (if slowly in the United States) to end these unnecessary procedures and bring awareness to these human rights violations, advocating for intersex people to make their own decisions about whether or not to have surgery or take hormones. At this time in the U.S., there are an unprecedented number of bills being proposed and passed across the nation targeting transgender and intersex people, children in particular, and their healthcare.
For centuries, Western medicine has debated which characteristics determine “true”/”biological” sex, breaking apart the very binary their research sought to prove. As a result of medical advancements in fields such as biopsy, endocrinology, anesthesia, and surgery over the last few hundred years, many intersex people have been and continue to be harmed or die at the hands of doctors. The standards for which sex determination are based are a hyper-idealized binary of a penis (defined by the ability to adequately penetrate a vagina) and a vagina (defined by the reverse) that are constructed — often quite literally through one or more surgeries — by a medical profession that has historically been dominated by White men. Standards that are influenced by the world around it, namely White supremacy, hetero- and cissexism, and colonialism.
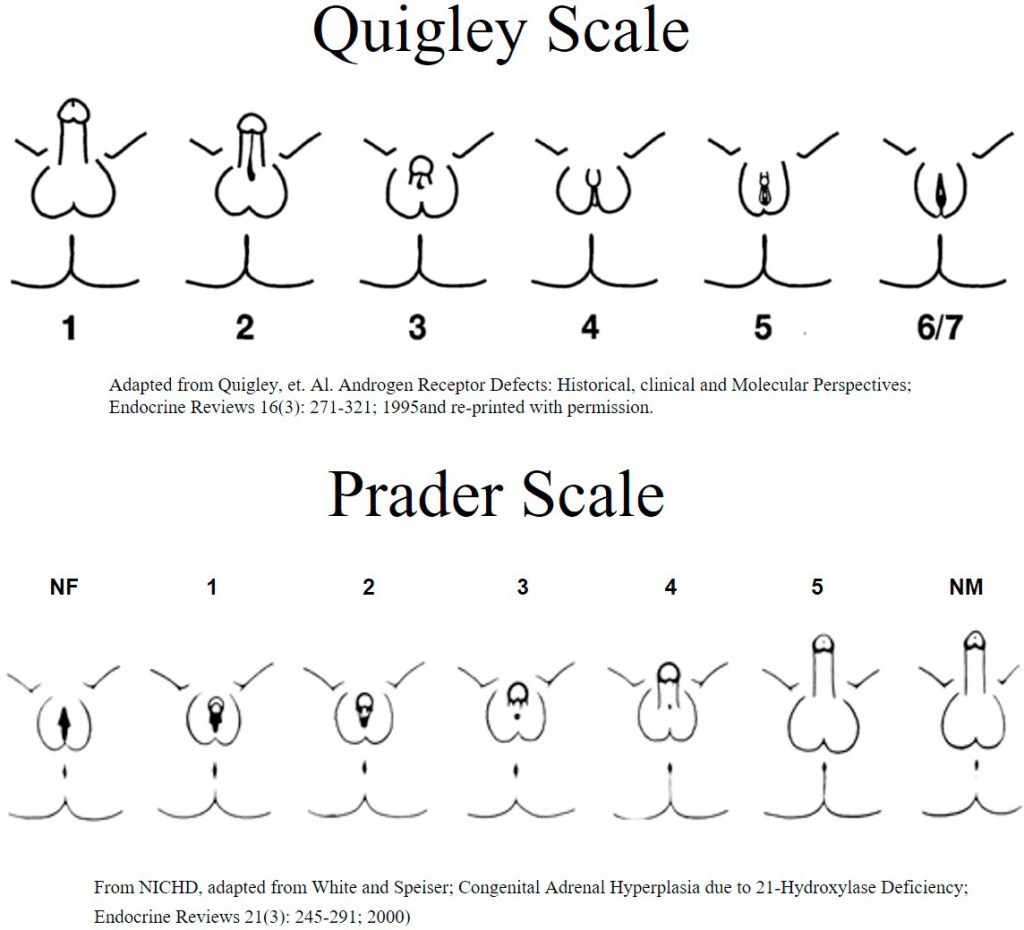
The lack of information about intersex people in sex, science, and health education is an act of erasure that perpetuates the notion of two “biological” sexes and pathologizes normal human variation; this is often echoed in popular culture where intersex people, if ever represented, are used for humor or shock value. As a result, a few problematic illustrations have become the “standard,” namely the highly criticized Prader scale, Quigley scale, and orchidometer, all clinical measurement tools that depict oversimplified line drawings of infant genitals. While generalizations in medical illustration are helpful to show commonalities across a group, it is inappropriate to use such images as a basis for surgical intervention.
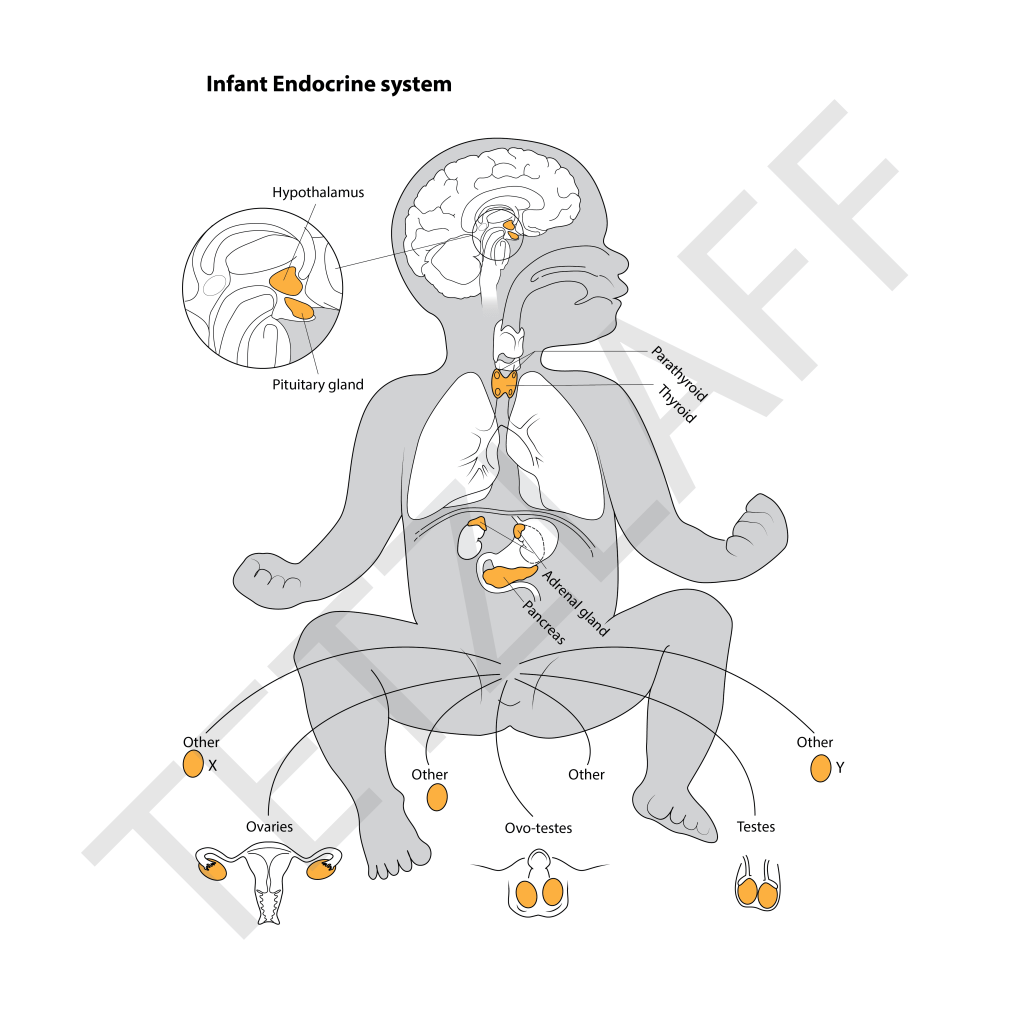
Sometimes including genitalia (intersex or otherwise) in education materials about infant/child health is simply unnecessary and/or distracting, making it a less effective learning tool. Many of the illustrations currently in medical textbooks are inaccurate, often just simplified versions of adult anatomy shrunk to fit. As all genitals change shape throughout the lifespan from ~6 months after birth, through adolescence and puberty, and across adulthood, it is incorrect to use male- and female-typical adult versions as a stand-in for reality. Furthermore, is it often not necessary to highlight the differences external differences of an infant for educational purposes, as testes, ovaries, and ovo-testes are internal or close to the body.
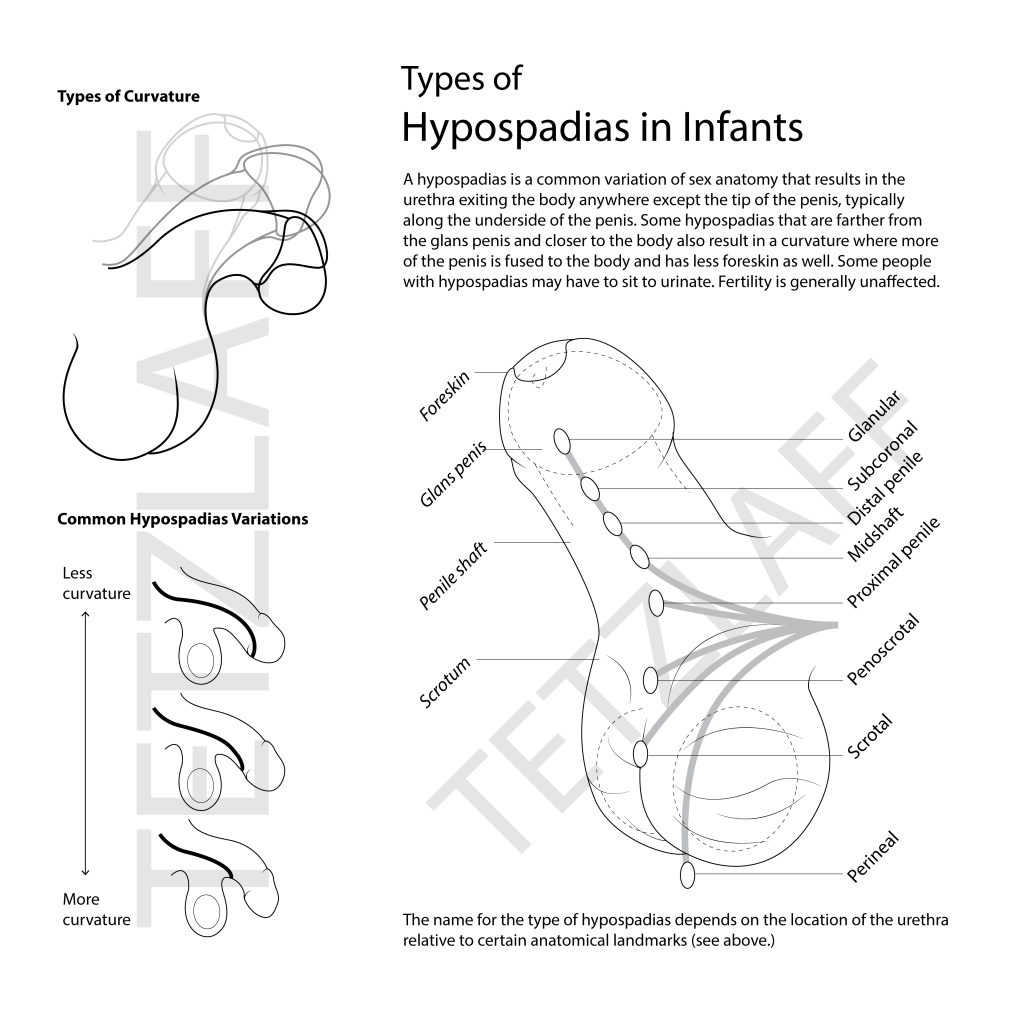
Hypospadia
A very common intersex characteristic is hypospadia, where the urethra (the tube that connects to the bladder) exits the body anywhere except the tip of the penis.